Santé
Primary Care
|
Strengthening primary care, and getting greater value out of this sector, is a priority for all OECD health systems. Primary care is defined as the first level of contact for the population with the healthcare system, bringing healthcare as close as possible to where people live and work. It addresses the main health problems in the community, providing preventive, curative and rehabilitative services. Primary care goes beyond services provided by primary care physicians to encompass other health professionals such as nurses, pharmacists, auxiliaries, and community health workers. Primary care as the first point of care, where primary care providers deliver people-centred care, has the potential to respond to major health challenges and to promote health for all. |
|
Strengthening the frontline: How primary healthcare helps health systems adapt during the COVID-19 pandemic - POLICY BRIEF
 |
Health systems continue to adapt to cope with the COVID-19 pandemic. Much focus has been placed on the scaling-up of hospital capacities. However, the pandemic is also deeply affecting the health of many people who are not infected by the virus. People living with chronic conditions are not only highly vulnerable to complications and death from COVID-19, but they are also suffering from disruptions to their regular care routines. The COVID-19 crisis demonstrates the importance of placing primary healthcare at the core of health systems, both to manage an unexpected surge of demand and to maintain continuity of care for all. Strong primary healthcare – organised in multi-disciplinary teams and with innovative roles for health professionals, integrated with community health services, equipped with digital technology, and working with well-designed incentives – helps deliver a successful health system response. Download the Brief (released 10 February 2021) Visit the dedicated webpage of the Organisation http://www.oecd.org/coronavirus/ |
Realising the Potential of Primary HealthCare
The OECD Health Division has an ongoing programme of work to support countries in strengthening primary care systems that can meet the needs of their populations now and in the future.
 |
The report Realising the Potential of Primary Health Care, released on 2 June 2020, discusses how primary care needs to evolve to meet the challenges that OECD healthcare systems – and societies more broadly – are facing, and identifying what high performing primary care will look like ten or twenty years from now. The report in particular identifies which countries appear to be at the leading edge of practice and share example of interesting innovations on how primary care systems can contribute to population health and society goals. Four major themes that dominate many policy agendas are explored:
Download the report Realising the Potential of Primary Health Care (June 2020) |
the Full Potential of Primary HealthCare - Policy Brief
 |
Released 16 May 2019. This brief has been produced to support discussions among G7 Health Ministers at their meeting in Paris, France, on 17-18 May 2019. As societies age and the burden of chronic disease grows, people need care that is centred on increasingly complex care needs, co-ordinated across the care pathway, and accessible (financially, geographically and around the clock). This makes good primary healthcare ever more vital. This Policy Brief provides a broad overview of the main policy issues and some of the policy actions that policy makers can put in place to strengthen primary healthcare.
|
PRIMARY CARE SPENDING
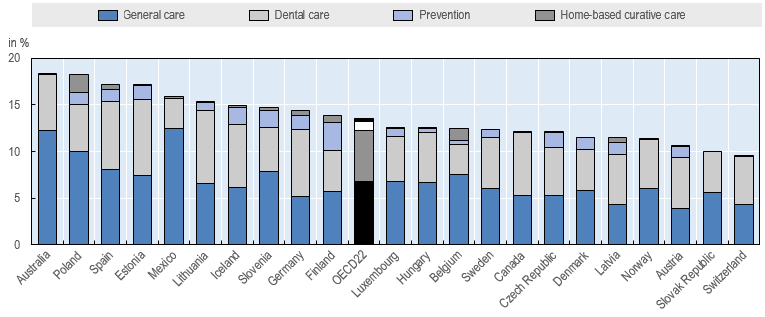
Spending on primary care services, defined as a set of basic care services provided outside of the hospital sector, accounted for an average of 14% of all healthcare spending across OECD countries in 2016. The share of spending on primary care services was highest in Australia and Poland (both 18%), followed by Spain and Estonia (both 17%). The Slovak Republic and Switzerland, on the other hand, only dedicated around 10% of their total health expenditure on primary care services.
- Read the paper Deriving Preliminary Estimates of Primary Care Spending under the SHA 2011 Framework (March 2019)
- Read the Policy Brief Spending on Primary Care: First Estimates (December 2018)
Spending on primary care services as share of total health spending among 22 OECD countries, 2016
Source: OECD Health Statistics 2023.
Access the data behind the graph.
The Patient-Reported Indicators Survey (PaRIS) initiative
|
Health systems know very little about whether the healthcare delivered seeks to improve people’s well-being and their ability to play an active role in society. It is only when we measure outcomes reported by patients themselves – such as quality of life – that important differences in the outcomes of care emerge. The OECD Patient-Reported Indicators Survey (PaRIS) initiative addresses these critical information gaps and aims to develop international benchmarks of health system performance as reported by patients themselves, and includes a focus on collecting the experiences and outcomes of users of mental healthcare services. In areas where patient-reported indicators already exist, the OECD supports countries to accelerate the adoption and reporting of validated, standardised, internationally-comparable patient-reported indicators. A working group on patient-reported indicators for mental healthcare is one of three international working groups that started in 2018, to discuss and coordinate instruments, definitions and data collection strategies across countries. In addition, a new set of internationally comparable measures will be developed to help policy makers assess to what extent their policies are on track to make health systems more people-centred, under the OECD Patient-Reported Indicators Survey (PaRIS) initiative. This new international survey focuses on patients with one or more chronic conditions, including mental health conditions such as depression or anxiety, who are living in the community and who are largely treated in primary care or other ambulatory care settings.
|
FURTHER READING
- Value-based payment models in primary care: An assessment of the Menzis Shared Savings programme in the Netherlands, OECD Health Working Paper No. 157
- Primary Health Care for Resilient Health Systems in Latin America, December 2022
- Health for the People, by the People - Building People-centred Health Systems, December 2021
- Primary Health Care in Brazil, December 2021 - also available in Portuguese: Estudo da OCDE da Atenção Primária à Saúde no Brasil
- Realising the Potential of Primary Health Care, June 2020
- Realising the Full Potential of Primary Health Care, Policy Brief, May 2019
- The Economics of Patient Safety in Primary and Ambulatory Care - Flying Blind, November 2018
- Caring for Quality in Health: Lessons Learnt from 15 Reviews of Health Care Quality, January 2017
- The organisation of out-of-hours primary care in OECD countries, OECD Health Working Paper No. 89
- Emergency Care Services: Trends, Drivers and Interventions to Manage the Demand, OECD Health Working Paper No. 83
- Health Statistics
- Health Working Papers
CONTACT US
For more information, please contact Ms Caroline Berchet: caroline.berchet@oecd.org

Follow us on Twitter @OECD_Social
Documents connexes